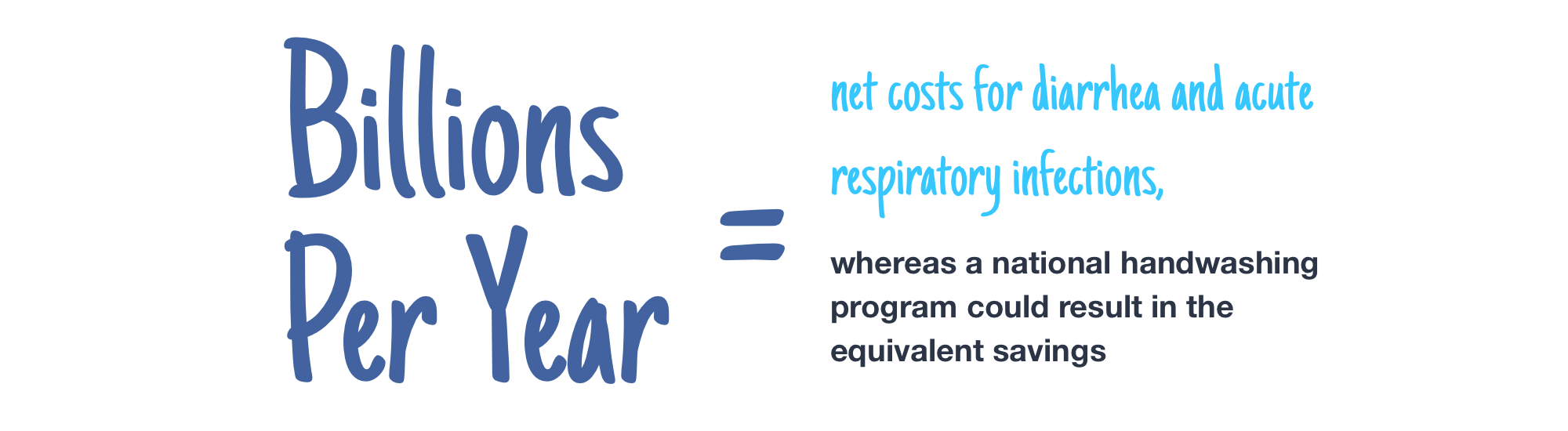Diarrheal Disease Solutions
WASH
Poor access to water, sanitation, and hygiene—collectively known as WASH—is responsible for more than half of diarrhea cases . Exposure to enteric pathogens in the environment due to poor WASH can lead to long-term gut damage, compromising a child’s physical and cognitive growth.
Though fewer children are dying from diarrhea today than ever before, unpredictable weather extremes due to climate change threaten to worsen infectious diseases like diarrhea. Too much or too little water spells danger for children and families, especially in crowded settlements.
WASH in institutional settings, such as health centers and schools, is critically important and is generally agreed to be one of the key integrated interventions for preventing infectious disease, stunting, and drug resistance. Health facilities, like diarrhea wards, are an especially crucial setting for improving WASH because of the risk of spreading infections. According to WHO and UNICEF , nearly 2 billion people use facilities that lack basic water services and nearly 800 million use facilities with no toilets.
– Dr. Tedros Adhanom Ghebreyesus, Director-General, World Health Organization (WHO)
in a WHO statement
– Stephen Luby, lead of the groundbreaking WASH Benefits Study in Bangladesh.
-
Problem: contaminated, unsafe water, or inadequate supply
This problem is critical in sub-Saharan Africa and Southeast Asia. Rural and poor communities lack infrastructure that ensures safe drinking water, while rapid urbanization is putting new pressures on flawed water systems.
Climate change is an exacerbating factor. Droughts can dry up water sources, leading people to use any water they can find, even if highly contaminated, and floods can contaminate water sources when the surge stresses infrastructure, including poorly constructed toilets.
Water can be contaminated at its source, during transportation, or at the point of consumption. Drinking or using unsafe water for washing, cooking, cleaning, or farming can lead to illnesses. This burden, and the constant search for a water supply, even when unsafe, falls most heavily on girls and women.
-
Solution: make water safe, address local needs
Solutions that make water safe must be tailored to meet local needs. Education and behavior-change tactics are also important to sustainability. Point-of-use and household water treatment and storage involve disinfecting water before it is used or consumed. There are a range of proven, low-cost methods, including disinfection by sun, UV lamps, boiling, filtration, and absorption, as well as chemical disinfection with chlorine, bleach, and flocculants. Innovation to address unsafe water may be as specific as an adapter ring in a water filter that accommodates several sizes of ceramic pots, or a design upgrade that encourages use. Once water is treated, it must be stored safely to prevent subsequent contamination.
Engagement with the private sector can help, too.
Everything from direct sales of water filters to automated water kiosks and ATMs may change the landscape of water providers. Learn more:Water filters:
Kiosks:
-
Impact: infections prevented, lives saved
If everyone had access to safe water, almost 90 percent of diarrheal deaths could be prevented.
-
Global guidance: water
The Sustainable Development Goals (SDGs), launched in 2015, include a target to ensure everyone has access to safe water by 2030.
Goal 6: Ensure availability and sustainable management of water and sanitation for all.
6.1: Achieve universal and equitable access to safe and affordable drinking water.
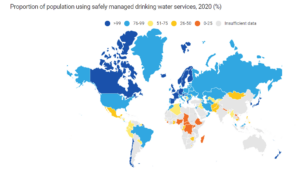
6.1.1: Proportion of population using safely managed drinking water services. Learn more.
WHO’s guidelines on drinking water quality provide the basis for national regulations and standards for water safety in support of public health.
The latest guidelines for drinking water quality can be found here.
Sanitation
Safely collecting, treating, and disposing of human waste reduces exposure to the causes of waterborne disease.
– Bill Gates, Co-Chair, Bill & Melinda Gates Foundation
in Gates Notes
-
Problem: lack of sanitation exposes people to infectious diseases
Billions of people do not have basic sanitation facilities, such as toilets or latrines, and defecate in the open in fields, streets, gutters, or open bodies of water.
Lack of basic sanitation (e.g., open defecation) creates serious health risks, including endemic diarrhea and the spread of diseases like cholera, diarrhea, and dysentery. It is also linked to transmission of hepatitis A, typhoid, and polio. In 2020, 494 million people still practiced open defecation.
Lack of sanitation access fuels the spread of infectious diseases like cholera, diarrhea, and typhoid, and a
total community approach to sanitation coverage is needed to prevent outbreaks.
The lack of access to basic sanitation facilities can also have serious safety implications, especially for women at night, and undermine feelings of self-dignity.
The vast majority of people without access to proper sanitation live in sub-Saharan Africa, East Asia, and South Asia. Unless addressed, the problem will only continue, with rapid urbanization and climate change presenting growing threats.
-
Solution: safely dispose of human waste
Proper sanitation means that people are separated from and do not come into contact with human waste. There is no “one size fits all” approach; the right intervention depends on the community’s needs, culture, and environment. Squat pan or seated pour-flush toilets, onsite biodigesters, or public latrine blocks are all appropriate for varying contexts.
As the world contends with climate change and rapid urbanization, sanitation access must be universal, flexible, affordable, and sustainable.

-
Impact: infections prevented, lives saved
Sanitation could substantially reduce diarrheal disease frequency and malnutrition indicators. Safely disposing of human waste impacts not only health, but also social and economic development.
Durability, privacy, and security
These were among the key user requirements for a joint Population Services International (PSI) and PATH sanitation project in rural India. The collaboration helped build a market for the sale of 150,000 toilets that are designed to be cost-effective and user-friendly. Addressing supply chain challenges, creating user-centered designs, and providing financing options for families to purchase their own toilets have been core components in the program’s success in Bihar.
-
Global Guidance: sanitation
The SDGs call for progress in sanitation by 2030:
Goal 6: Ensure availability and sustainable management of water and sanitation for all.
6.2: Achieve access to adequate and equitable sanitation and hygiene, and end open defecation, paying special attention to the needs of women, girls, and those in vulnerable situations.
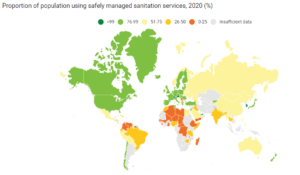
6.2.1: Proportion of population using safely managed sanitation services, including a handwashing facility with soap and water. Learn more.
WHO Joint Monitoring Programme (JMP) Report: Progress on household drinking-water, sanitation and hygiene: Five years into the SDGs:
This 2021 report extrapolates estimates based on existing trends to illustrate current trajectories and the acceleration required to achieve universal WASH coverage by 2030. Learn more.African Sanitation Policy Guidelines:
This resource gives African governments guidance for enhancing or developing clear and comprehensive national sanitation policies and programs. Learn more.
Hygiene
Handwashing with soap is a simple and effective way to prevent diarrhea. Hygienic practices like handwashing maintain health and prevent the transmission of diseases.
-
Problem: limited access to soap and water, knowledge, or good hygiene practices
Contaminated hands are one of the main ways diarrhea is spread. In 2020, 2.3 billion people lacked access to basic hygiene services at home; 818 million children lacked handwashing services at school; and one in three health facilities lacked handwashing stations at points of care.
-
Solution: handwashing with soap can prevent the transmission of illnesses
Since diarrheal diseases are transmitted through the fecal-oral route, routine handwashing with soap can prevent the transmission of the bacteria and viruses that cause diarrhea, particularly when regularly practiced after using the toilet or changing a baby’s diaper and before preparing food.
Handwashing with soap is one of the most cost-effective investments in public health. Handwashing prevents diarrhea and a host of other infections that can be extremely costly to individuals, health care systems, and countries.
Washing hands in schools and health care facilities can have a significant impact.
It is critical to educate both parents and caregivers on the importance of correctly washing hands. For children, schools provide ample opportunities for promoting healthy habits.
Since improving handwashing requires behavior change, it works best as part of a broader package of solutions.

-
Impact: infections prevented, lives saved
Handwashing with soap could eliminate nearly half of all diarrhea infections.
Without good hygiene practices like handwashing with soap, efforts to improve drinking water and sanitation will be undermined and unsustainable. The SDGs are monitoring the percentage of people with facilities in their homes to wash their hands with soap and water. Access varies immensely, from 15 percent of the population in sub-Saharan Africa to 76 percent in West Asia and North Africa.
Further reading:
- DefeatDD. How does soap actually work?
- DefeatDD. Solutions: WASH.
- Global Handwashing Day.
- UNICEF. Progress on household drinking water, sanitation and hygiene, 2000-2020.
- UNICEF. Water, sanitation and hygiene (WASH).
- United Nations. Sustainable Development Goal 6.
- WASH in Health Care Facilities.
- WaterAid. Caught short: how a lack of access to clean water and decent toilets plays a major role in child stunting.
- World Water Day.